Researchers: WHO guidelines are unattainable in poor countries
What do you do in a country like Tanzania, for example, when the WHO says that all countries must set up COVID centers?
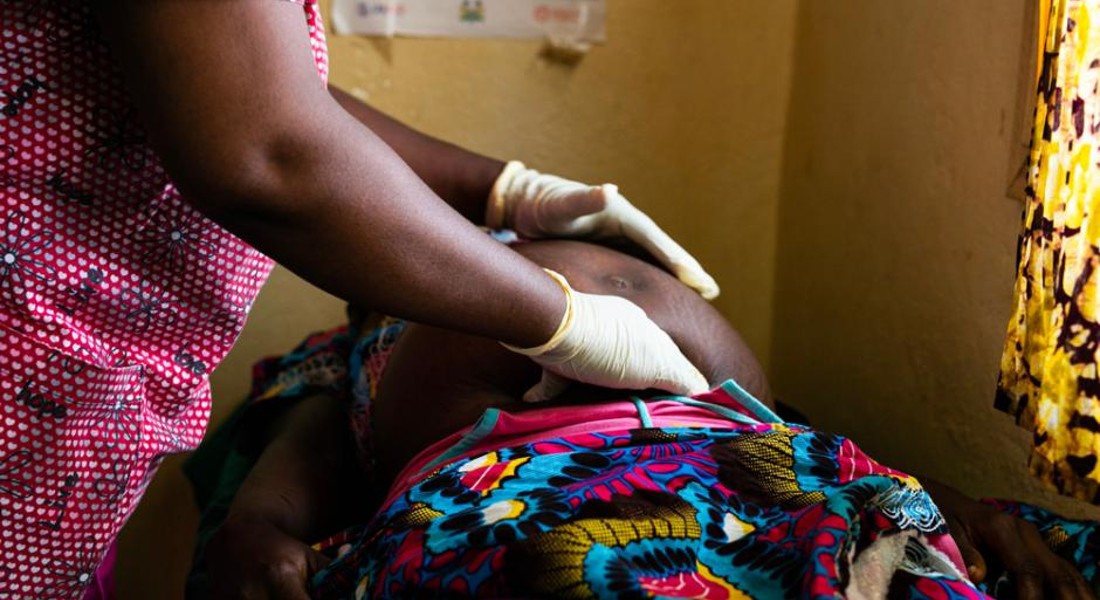
The World Health Organization’s (WHO) guidelines are being rolled out worldwide with the aim of ensuring the best and most evidence-based treatment for all people.
But many of the recommendations are so far from the reality in low- and middle-income countries that they cannot be used and in worst case scenarios can cost lives.
"WHO is the world’s health organization but their guidelines are very much based on studies and expert consensus from high-income countries - a reality that is so far from the reality in poorer countries, which often make these guidelines completely unattainable" says postdoc at the Global Health Section, University of Copenhagen, Nanna Maaløe.
And it is a huge problem that ultimately can cost lives in the poorest countries, writes Nanna Maaløe and a number of other researchers from Denmark, Tanzania, Burundi and the Netherlands in a Viewpoint article in the Lancet Global Health.
“Most often, just one version of guidelines is developed for everyone in the world, without subsequent evaluation of whether the guidelines have had the desired effect when they hit the front line of poor health systems. And regionally and nationally in low- and middle-income countries, resources are often not prioritized to modify these guidelines to reality, which is why unattainable guidelines are rolled out" says Nanna Maaløe.
In her opinion, WHO guidelines should be evaluated to a greater extent in the same way as medicines.
"Medicines undergo clear phases of testing before and after the roll-out of both efficacy and side effects. However, clinical guidelines that, among other things, recommend when medicines should be used are often rolled out without pilot testing or later evaluation."
In addition to being a researcher, Nanna Maaløe is also a doctor at Hvidovre Hospital, and she has made studies of how to co-develop local guidelines at maternity clinics in Tanzania.
Labor inducting medicines can be dangerous in Africa
But wait a minute. After all, medicines can have side effects, and therefore they must be tested very thoroughly. But a piece of paper from the WHO with good advice on how a doctor approaches the treatment - how should this be able to have unexpected effects?
A good example of how the problem can arise are guidelines in relation to the labor inducting medicine, oxytocin:
Labor inducting medicine can trigger a birth that has stalled and where the unborn baby risks an oxygen deficiency if it does not come out soon. It is one of the most frequent treatments during childbirth worldwide.
"But the same medicine can be dangerous and is classified as 'high-alert medication', i.e., medicine with a particularly high risk of damage, not least if the obstetrician cannot keep a sufficient eye on the mother. The medicine can cause such strong labor that the contractions close the oxygen supply through the umbilical cord to the fetus," says Nanna Maaløe.
Therefore, the WHO's guidelines for obstetricians state that if a birth stops, you must give it some time in an unspecified period of time, and subsequently you can advantageously give labor inducting medication. But that it is important to dose the amount very carefully and keep a close eye on the mother.
"It is individual how large a dose each individual needs. At Hvidovre Hospital, we have electronic drop counters. But you just do not have that in public hospitals in Tanzania, for example. And here, one midwife must often handle 5-6 women giving birth at the same time," says Nanna Maaløe.
She says that there are also studies from our part of the world that show that it is risky to use this labor inducting medication, and therefore many measures are taken to ensure an optimal dosage.
And Monica Kujabi, Nanna Maaløe's PhD student, is currently completing a systematic review and meta-analysis of the literature from low- and middle-income countries, which is worrying.
"In low-resource countries, our meta-analysis shows that labour inducting medication with oxytocin is related to stillbirths and severe oxygen deficiency at birth," says Nanna Maaløe.
Thus, labor inducting medication is most often a good treatment in Denmark, for example, while in Tanzania in certain situations it may be better to do without.
The use of labor inducting medication is just one example where the WHO health guidelines do not take into account the reality outside a well-equipped western hospital.
Reality is far from RCT studies
When the WHO makes its guidelines, it is based on a classical understanding of health science, where so-called randomized controlled trial (RCT) studies (lottery experiments, which are the golden standard in health science methods) and meta-studies (overview studies) give the strongest research results.
An RCT study is testing a treatment - for example labour inducting medication - in a group of patients, who are drawn by lottery to either receive active treatments or placebo.
Then you can assess whether the medicine works and what side effects it may have. In this way, for example, it has been found that labor inducting medication is probably better than nothing if a birth stops. But also that the patient must be closely monitored.
"The reality in which RCT studies are usually made is so far from the reality in many low-resource hospitals that it is often challenging to conclude something about the effect in places where, for example, the lack of resources comes into play," says Nanna Maaløe.
The WHO is in fact in the process of re-evaluating the starting point of their guidelines and has recognized that more evaluation and other information is needed as well. For example, the resources, cultural and social aspects of the health system
But they also acknowledge that they are far from achieving the goal of better guidelines, two WHO representatives write in a comment in the Lancet Global Health from 2017.
5 women giving birth per obstetrician
One time, in connection with her research in Tanzania, Nanna Maaløe worked in a maternity clinic in the countryside. She spoke to the midwife at the clinic about WHO's guidelines.
"I remember her saying: ‘That book is not made for me.’ Simply because her reality was completely different and could not be accommodated in the WHO guidelines."
For example, the WHO recommends that contractions should be monitored every half hour for 10 minutes when a woman is in labor.
“But if you are one midwife for 5-6 women giving birth, then you cannot attend them for 10 minutes each. The problem is that when the recommendations are so far from reality, people become completely powerless and may not monitor at all," says Nanna Maaløe.
According to Nanna Maaløe and her research colleagues, it would be beneficial that the WHO, in collaboration with local governments and health professionals, made some more contextual guidelines.
“For example, we know that it is important to listen often to the heart sound of the unborn child during a birth. Then one could have guidelines that said that if there are enough staff, one should do the optimum and listen every 15 minutes. If you are too few, you can reduce and say every half hour, or every hour. It is not optimal, but it is better than nothing, «says Nanna Maaløe.
Maternity clinics transformed into COVID centers
Another example Nanna Maaløe mentions is the WHO's guidelines in connection with the corona pandemic.
Here, the WHO recommended all countries to set up special COVID centers or COVID wards for corona infected people. But at the same time, the organization stressed that all essential functions of the health care system should be maintained.
“The problem is that some low-income countries did not even have the resources to maintain the most necessary essential functions. When they had to set up COVID centers, even more essential functions disappeared, «says Nanna Maaløe.
She mentions that in Tanzania, for example, a large maternity clinic in the capital was closed within just three days' notice to set up a COVID center. At the clinic, more than 12,000 women give birth annually. There was no plan for where the rejected women should give birth instead.
Lacking local adaptation
Associate Professor in Epidemiology at the University of Southern Denmark, Ane Fisker, can to a large extent recognize the challenges of lacking local adaptation and lacking follow-up on whether measures and guidelines actually work as intended in poorer countries.
She is researching the implementation of childhood vaccination programs and other health services in Guinea Bissau in West Africa.
Here, health checks of pregnant women have been introduced. Four times in total, pregnant women must pass the local health clinic and be checked.
The effect is measured in accordance with WHO's guidelines, by counting how large a proportion of pregnant women have time to get all four checks. The goal is for 80 percent to be checked 4 times.
“The problem is that if a heavily pregnant woman has not been for a check-up before, but shows up at the health clinic to be checked, then she will often be rejected. Simply because she will count negatively in the statistics. This is an example of organizing the evaluation so that it measures how many receive optimal treatment. But this means that those who do not have the opportunity for the optimal treatment end up not receiving any treatment at all" says Ane Fisker.
In her opinion, an unfortunate consequence of unrealistic guidelines and too much focus on evaluation is that the focus shifts from what can actually be done.
A and B standards for treatment?
It is a great challenge to balance between which treatment is the best in an optimal reality and what is the realistic treatment.
This is what Rebecca Nantanda says, who researches lung health in children, among other things, at Makerere University Lung Institute in Uganda.
"WHO guidelines should help healthcare professionals provide the best treatment. Guidelines focus on ensuring that as many people as possible survive. For example, we know that guidelines in relation to assessing sick children mean that virtually all children with pneumonia are detected. Guidelines are important in a country like Uganda, which has problems with diagnosis and where many children are still dying” she says.
She is backed by her research colleague Peter Waiswa, who is an Associate Professor of health policy and planning at Makerere University School of Public Health, College of Health Sciences in Uganda.
“It is clearly a challenge for WHO guidelines to fully adapt to local conditions, as the context can vary widely. WHO guidelines are always and rightly so general. In individual countries, the WHO should work with national governments to ensure that these guidelines come closer to the reality in which people live and work. I really hope they have learned that from COVID-19,” he says.
WHO guidelines do not have to be abandoned
In Rebecca Nantanda's opinion, WHO guidelines can be used as a guide for optimizing treatment in low-income countries in the right direction and improving the health system towards the best treatment.
In the opinion of the two researchers, it is important not to abandon the idea of letting the best research guide treatment even in low-income countries.
“These guidelines are based on the best research. But implementing them can be a challenge. Still, we should do everything we can to ensure that they are made usable everywhere, so that all children can benefit from the best research, whether they live in high-income or low-income countries, ” emphasizes Rebecca Nantanda.
Nanna Maaløe completely agrees with this.
“The treatment recommended by the WHO is perhaps rationally the best imaginable. But it is not the best in all realities. However, this is a very sensitive subject, and I agree that it is ethically challenging to present different standards for different levels of resources" says Nanna Maaløe.
"But for the nurse, the midwife and the doctor who work at a low-resource hospital, it is extremely important that they can actually get help from these guidelines," she emphasizes.
If one dares to face the realities and make guidelines that realistically fit different realities, it may in her eyes help to focus on the extremely great inequality that exists.
"Health care providers at the forefront of the world's health systems are crucial to achieving the health-related sustainable development goals - and these doctors, nurses and midwives need relevant and achievable clinical guidelines to cope with their overworked work, day and night" emphasizes Nanna Maaløe.
Sources
- Nanna Maaløe's profile (KU)
- Ane Fisker's profile (SDU)
- Rebecca Nantanda's profile (Makerere University)
- Peter Waiswa's profile (Makerere University)
- The injustice of unfit clinical practice guidelines in low-resource realities, The Lancet Global Health 2021, DOI:https://doi.org/10.1016/S2214-109X(21)00059-0
